If you’re dealing with urinary problems, a weird change in your flow, or that nagging feeling of prostate discomfort, you’re not “overthinking it.” You’re noticing signals from a very small organ that can cause very big disruption.
I’ve seen the same pattern again and again in clinic style conversations: a patient waits months because the symptoms feel “embarrassing,” then shows up exhausted from waking up at night to pee, frustrated by a weak stream, and worried it might be cancer. The truth is simpler and more useful: many prostate problems are benign and treatable, but you need the right workup to separate a benign issue from something serious.
This guide explains what the prostate is, why “weak prostate muscles” can affect urination and ejaculation, which prostate issues symptoms matter most, what diagnostic tests actually determine the cause, and when to see a urologist in Dubai.
First, what is the prostate and why does it cause so much trouble?
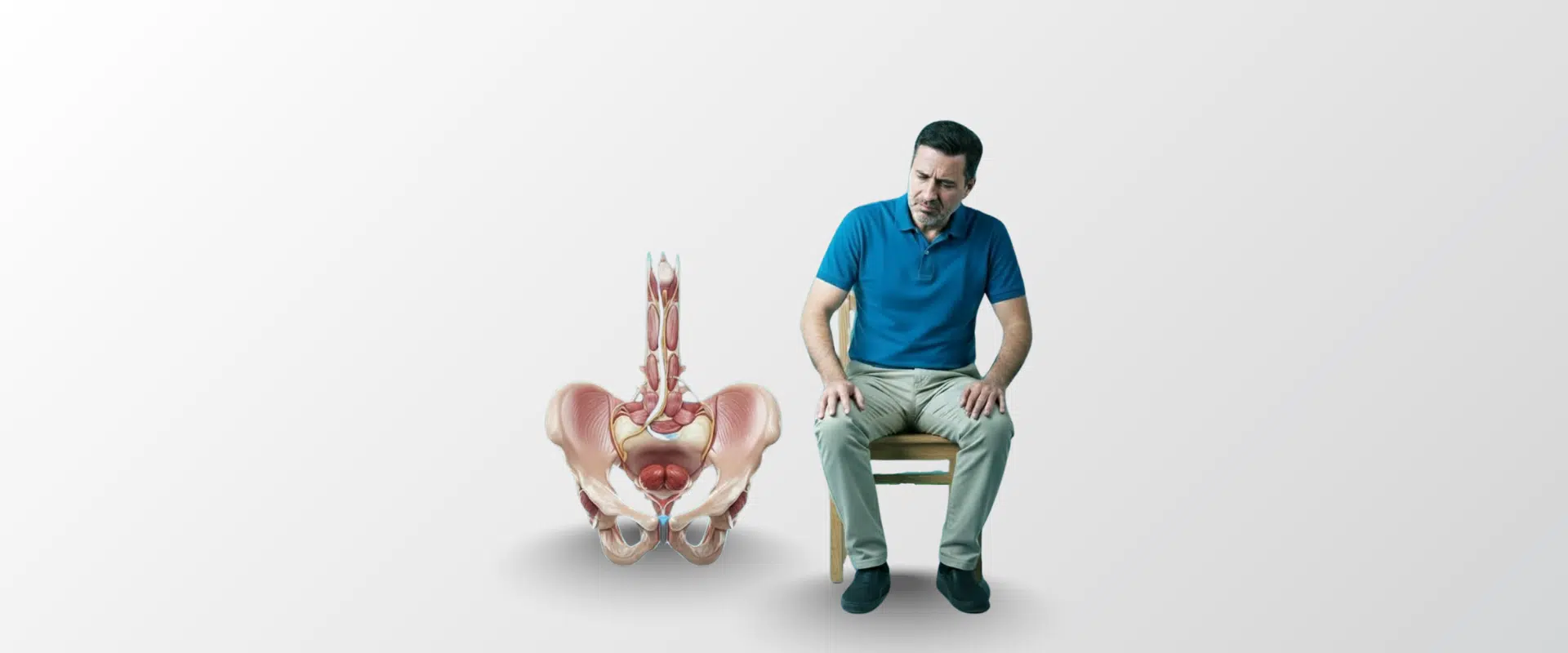
The prostate is a small gland in the male reproductive system. In your 20s, it’s usually normal walnut size. As age increases, it may become grown and slightly larger around ages 40, and in many men by 60 it can reach something closer to a lemon in overall bulk. That growth can raise risk for prostate problems like BPH or benign prostatic hyperplasia.
Location is the key to understanding symptoms: the prostate sits under the bladder, in front of the rectum, and it surrounds the urethra, the tube that carries urine through the penis. So when the prostate swells or enlarges, it can squeeze the urethra like a clamp.
Function-wise, the prostate helps make semen, adding a white, milky fluid that mixes with sperm. During orgasm, muscles in and around the prostate push fluid during ejaculation.
So yes, “weak prostate muscles” is a real concept in everyday terms, but most of the time what people feel as “weak” is actually a mix of:
- prostate-related blockage (flow is weak because the urethra is squeezed), and or
- bladder muscle strain (the bladder has to work harder against resistance), and or
- pelvic floor coordination issues (common with anxiety, chronic pain, long sitting, and sometimes after inflammation).
The symptom patterns that point to prostate problems
Here’s a simple way I explain it: symptoms usually fall into “flow,” “irritation,” “pain,” and “red flags.”
Quick table: symptoms and what they often suggest
| What you notice | Commonly linked to | Why it happens |
|---|---|---|
| frequent urination, sudden need to urinate, urgency | BPH, irritation, infection | Bladder gets overactive or feels “full” early |
| Waking at night to pee | BPH, fluids/caffeine timing, bladder overactivity | Less bladder “reserve” or more nighttime production |
| difficulty starting, stop-start flow | BPH or inflammation | Urethra compressed or irritated |
| weak stream, dribbling | BPH, bladder strain | Resistance at prostate level |
| pain, burning while urinating | UTI, prostatitis | Inflammation or infection |
| blood in urine or semen | Needs evaluation | Can be infection, stones, enlarged vessels, or cancer |
| painful ejaculation | Prostatitis, pelvic pain syndrome | Inflamed tissues or pelvic floor spasm |
“Weak prostate muscles”: what people mean vs what’s happening
When patients say “my prostate muscles are weak,” they usually mean one of these lived experiences:
- The urine stream feels thin and powerless
- It takes effort to start
- They strain, then still feel the bladder isn’t empty
- Ejaculation feels less forceful, or is painful
Here’s the blunt truth: the prostate itself is not a gym muscle you can “strength train” directly. What you can improve is the system around it, once you know the cause.
- If it’s benign prostatic hyperplasia (BPH), the main problem is tissue overgrowth and compression, so treatment focuses on relaxing or shrinking the prostate and reducing obstruction.
- If it’s prostatitis or chronic pelvic pain, the target is inflammation, infection (when present), and pelvic floor over-tension.
- If it’s bladder strain from long-term obstruction, the plan is to remove the obstruction and retrain bladder habits.
What is a prostate?
The prostate is a small, firm, partly muscular gland that helps make fluid for the male reproductive system. It surrounds part of the urethra and contributes to the fluid that becomes semen.
Where is the prostate located?
Below the bladder and in front of the rectum.
What does it look like?
In early adulthood it’s typically walnut size. With age it often becomes grown and slightly larger, sometimes approaching lemon size in older ages.
What does the prostate do for a man?
It adds fluid that helps form semen and its muscles help propel fluid during ejaculation. It also makes proteins like prostate-specific antigen (PSA) that influence semen consistency.
The three most common prostate problems (and how they differ)
What is prostatitis?
prostatitis is a benign condition involving inflammation of the prostate. It can happen with or without a bacterial infection, and it can raise a PSA level, which is why you never want to panic from one lab result without context.
Types you should know:
- acute bacterial prostatitis: usually a bacterial infection, least common, symptoms can start suddenly and get worse quickly. Often includes fever, chills, body aches, nausea, vomiting, burning with urinating, frequent urgent need to urinate, difficulty, weak urine stream, and pain in lower belly/abdomen/groin/genitals/lower back. If you’re unable to urinate, seek treatment urgently.
- chronic bacterial prostatitis: repeated or lingering bacteria, similar but often less severe, can come and go over months, sometimes with urinary tract infections that keep returning.
- chronic pelvic pain syndrome: pain and urinary symptoms lasting 3 months or more, often no clear infection, commonly misunderstood.
- asymptomatic inflammatory prostatitis: no symptoms, white blood cells found on testing.
Important: prostatitis is not automatically prostate cancer, but it must be evaluated so you do not miss something serious.
What is benign prostatic hyperplasia (BPH)?
benign prostatic hyperplasia (BPH) is an enlarged prostate caused by increased cell number, and it is benign, meaning it’s not cancer. As the prostate enlarges, it can press against the urethra and affect the bladder’s ability to empty.
Common symptoms:
- needing to urinate often, especially at night
- pushing/straining to start
- weak/slow stream, dribbling
- stopping and starting multiple times
- feeling the bladder didn’t empty
- sometimes pain or issues around ejaculation
- sometimes blood in urine (always evaluate)
If untreated, severe obstruction can contribute to bladder weakness, infections, retention, and kidney issues.
What treatments actually do:
- alpha-blockers help relax muscles around the bladder neck and prostate to improve flow (symptom relief).
- 5-alpha reductase inhibitors help shrink the prostate over time and may take months.
- some men need minimally invasive procedures or surgery depending on severity and anatomy.
Also, don’t ignore lifestyle triggers that worsen symptoms, including alcohol and caffeine timing, and yes, sometimes bike riding can aggravate pelvic discomfort in sensitive cases.
What is prostate cancer?
prostate cancer is cancer that forms in prostate tissues. Risk rises with being older, certain genetic patterns, and family history. Early stages often have no symptoms, which is why testing is nuanced and needs shared decision-making.
Symptoms when more advanced can include urinary changes, blood in urine or semen, or persistent pain in back/hips/pelvis.
Screening reality check: the PSA test can help detect cancer early, but it also creates false alarms and can lead to overdiagnosis and unnecessary procedures. That’s why guidelines emphasize discussing benefits and harms before screening.
How doctors actually determine what’s going on
If you’re in Dubai and booking with Urologic Health Dubai, the goal is to quickly separate:
- infection (like urinary tract infection or bacterial prostatitis)
- obstruction (BPH)
- other urinary tract causes
- cancer risk that needs further evaluation
The core evaluation usually includes
- A careful symptom history (day vs night frequency, urgency, pain, sexual symptoms)
- A physical exam
- Often a digital rectal exam to check size, tenderness, nodules
- Urine testing and sometimes blood work, including prostate-specific antigen (PSA) when appropriate
- Depending on findings: imaging, uroflow testing, or referral for procedures
Practical table: common diagnostic tests and what they’re for
| Test | What it checks | Why it matters |
|---|---|---|
| urinalysis | infection markers, blood | Helps detect UTI and other issues |
| PSA test / PSA level | prostate-related protein in blood | Can rise in cancer, BPH, and prostatitis, guides next steps |
| digital rectal exam | size, tenderness, lumps | Flags suspicious findings, also prostatitis tenderness |
| Ultrasound or MRI (when needed) | anatomy, suspicious areas | Helps guide management, sometimes biopsy decisions |
| prostate biopsy (select cases) | tissue diagnosis | Confirms or rules out cancer |
If your PSA level is high, the right response is not panic. It is: repeat when appropriate, interpret in context, treat infection or inflammation if present, and decide on imaging or biopsy based on risk.
Red flags you should not ignore
Some symptoms mean “book soon,” others mean “go now.”
| Symptom | Action |
|---|---|
| Unable to pass urine, severe retention | Urgent same-day evaluation |
| fever, chills, severe pelvic or back pain with urinary symptoms | Urgent evaluation for acute infection |
| Visible blood in urine | Prompt medical evaluation |
| New severe pain, worsening symptoms rapidly | Don’t wait, get assessed |
Smart, low-risk steps that often help while you wait for assessment
These are not “cures.” They are practical symptom reducers that don’t block proper diagnosis:
- Reduce caffeine and alcohol, especially late evening (less irritation, fewer night trips).
- Don’t “just in case” pee every 10 minutes. That trains urgency. Use timed voiding instead.
- Hydrate earlier in the day, taper at night.
- Avoid long pressure sitting if pelvic pain is prominent (some patients flare with long rides like bike riding).
- If pain is present, don’t self-prescribe antibiotics. Get tested first so treatment matches cause.
Talk with your doctor about prostate health
If you have prostate issues symptoms, ask direct questions:
- Is this likely benign or suspicious?
- Which prostate tests do I actually need?
- Do I need a PSA test now, or later?
- What are the treatment options and side effects?
- What is my follow-up plan and timeline?
A urologist specializes in diagnosing and treating diseases of urinary organs in males and females, and manages prostate tests that check prostate problems properly.
Final reality check
Most men who worry about prostate problems end up with a benign explanation like prostatitis or BPH, but the symptoms overlap with serious conditions. If you want this handled professionally, the winning move is simple: stop guessing, get the correct diagnostic tests, and let a qualified doctor or urologist map out the plan.